
A common disorder affecting facial skin.
Initially carries both a vascular and an inflammatory component
– Inflammatory: Papules, pustules
– Vascular: Erythema, telangiectasia, flushing
Distribution
- Symmetrical localization on the face; may be asymmetrical
- Nose, cheeks, forehead, chin
- May involve a variety of ocular lesions
Etiology
- Unknown
- Age – thirty to fifty years at onset (most common);
- may occur from adolescence to late adult life
- Females predominate, but severity is greater in males
- Greater incidence in fair skinned people
Clinical Picture
- Flushing – periodic reddening of the face (erythema)
- Inflammatory lesions – papules, pustules
- Edema may be present
- Telangiectasia may be added with time
- Ocular rosacea – accompanies vascular cutaneous rosacea
- Comedones are characteristically absent
- Diagnosis is made on a clinical basis
- Rhinophyma is a late finding
Early Clues To Rosacea
- Recurrent flushing, blushing; may last several minutes – several hours
- Stinging in the malar areas, forehead, ears
- Facial edema may be present
Rosacea Often Progresses In The Following Steps
- Pre-rosacea ===> Flushing and blushing
- Vascular Rosacea ===> Erythema and telangiectasia
- Inflammatory Rosacea ===> Papules and pustules
- Late Rosacea ===> Rhinophyma
Facial Flushing
- Is a prominent feature of rosacea
- Is usually the initial manifestation of the disease
- Worsens during inflammatory outbreaks
- Patients should avoid activities and aggravating factors which induce flushing
Rhinophyma
- Enlargement of the nose
- More common in males
- Skin thickens
- Enlarged follicles
- Hyperplasia of sebaceous glands, connective tissue
Pathogenesis: Theories Proposed
- Demodex folliculorum
- Psychogenic stress
- Endocrine abnormalities
- Focal infection
- Vascular disorder
- Diet
Vascular Disorders
- Leaky vessels
- Insufficient blood flow
- “Pooling effect”
- Connective tissue dystrophy – leads to dilation of blood vessels
Rosacea – Aggravating Factors
- Hot liquids
- Sun exposure, wind exposure
- Spicy foods
- Extreme temperatures
- Alcoholic beverages
- Stress and other psychological factors
- Prolonged use of topical fluorinated corticosteroids
Differential Diagnosis
- Acne vulgaris
- Seborrheic dermatitis
- Perioral dermatitis
- Lupus erythematosus
- Carcinoid syndrome
- Some may exist
Course Of Rosacea
- Chronic, progressive disease
- Periodic exacerbations and remissions common
- May slowly increase in extent
- Inflammatory ocular complications may occur
- Long-term therapy may be required
Topical Steroids – Are Best Avoided
- Can cause rebound erythema
- Can worsen the condition in long run, although may effect impressive short-term improvement
- If used, should be low potency for short time period
Methods Of Treatment
- Oral antibiotics – tetracycline and others
- Topical formulations – metronidazole topical gel and others
- Many patients will do well with topical therapy alone.
- For some patients, the addition for oral tetracycline for several weeks may accelerate initial response to therapy.
- Lifestyle changes are also an important aspect of the overall treatment plan.
- Avoidance of situations and factors that aggravate rosacea should be emphasized.
Answers To Common Patient Questions
1. Question: I have very sensitive skin due to my rosacea. How can I clean my face without causing additional irritation?
- Answer: Only very mild soaps or mild cleansers should be used on the face. Avoid products containing alcohol or witch hazel.
2. Question : What about cosmetic use? Can I continue to wear cosmetics?
- Answer: Yes, but use of high quality mosturizers and oil-free cosmetic products are recommended. Sunscreens of SPF 15 or higher should be used when prolonged sun exposure is expected. To reduce the redness or a rosacea flare, a green-based concealer may be used.
3. Question: Can anything make rosacea worse?
- Answer: Certain things are known to aggravate rosacea. These include hot liquids, alcohol, spicy foods, extremes of temperature and stress.
Source of information: here

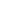

 +41 22 738 18 48
+41 22 738 18 48